What is rhinoplasty?
The nose remains a central key element in the context of your appearance. It is where our eyes often focus their attention. By changing the shape of the nose through rhinoplasty at our Westmead, Norwest, and North Shore practices, Dr Chaithan Reddy is able to address the overall appearance of the face.
Is rhinoplasty right for me?
A rhinoplasty procedure, sometimes referred to as a nasal reshaping procedure or a “nose job,” may be performed to correct nasal deformities resulting from trauma, or it may be performed to change the appearance of your nose. Whatever your reasons for undergoing the procedure, because of Dr Reddy’s extensive experience in nasal surgery and rhinoplasty over the past 15 years, he has confidence in producing, aesthetically pleasing results that address your concerns.
Am I a good candidate for rhinoplasty?
Through a rhinoplasty procedure, Dr Reddy can:

- Change the shape of your nose (define or refine)
- Change the size of your nose (augment or reduce)
- Correct a dorsal ‘hump’ or hook nose
- Change the width of your nostrils (reduce)
- Straighten a crooked nose
- Improve airflow through your nose
- Reconstruct a deficient nose
If you present with any of the above concerns, then you remain a suitable candidate for rhinoplasty surgery.
Your rhinoplasty may be performed at any one of our preferred private hospitals located in Sydney’s North Shore, Norwest, Western Sydney, and Central Coast regions. The procedure is performed using either an ‘open’ or ‘closed’ technique. The choice of technique will depend upon the existing shape of your nose and what is desired. Dr Reddy is proficient in both approaches, having learnt techniques from the world-renowned rhinoplasty surgeon, Dr Rolin Daniel. The aim of the first consultation with Dr Reddy will be to identify your current concerns and plan an operation that is tailored to your desires and your specific facial shape.
- Expert Advice
- Personal Approach
- Highly Respected
SYDNEY & CENTRAL COAST PLASTIC SURGEON

Our Surgery
Information Booklet
Fill out the form below to receive your copy of our surgery information booklet
Rhinoplasty procedure
The procedure is performed under a general anaesthesia. Once you are asleep Dr Reddy will mark out the planned incision (if ‘open rhinoplasty’). The nasal skin will be elevated, allowing the underlying framework to be reshaped. This will entail not only repositioning your nasal bones, but also altering the shape of your cartilages in order to produce a fine well-defined nose. Depending upon what was discussed at your pre-operative consultation, additional procedures directed at improving your breathing may also be performed at this time. Such procedures include a septoplasty procedure and or a turbinate reduction procedure. Other adjunctive nasal procedures include alar base narrowing or ‘sill’ reduction to address nostril flaring.
Upon completion of the rhinoplasty procedure and any of the aforementioned adjunctive procedures, skin closure is performed with delicate fine gauge sutures. A contoured nasal splint will be applied to your nose. If a septoplasty procedure was also undertaken, you will generally also have soft silicone internal nasal splints inserted. Cool packs will also be applied to your eyes for comfort.
What aspects of the nose can be altered?
There are various aspects of the nose that can be altered. The nose is made of various units, that describe the various parts of the nose. The main units of the nose that are frequently modified during rhinoplasty.
Include:
- The nasal tip
- The nasal bridge
- The nasal sidewalls
- The nostril rims
Addressing any of the above units of the nose typically involves modifying the nasal cartilages and nasal bones. If one is to consider the nasal tip, it is important to understand that it is made up of nasal cartilages.
The nasal tip can come in various shapes and sizes based on the shape and size of the underlying nasal cartilages. These cartilage pieces are referred to as the lower lateral cartilages. Depending upon the shape of these lower lateral cartilages, the nasal tip shape can vary.
Common nasal tip shapes include:
- Round nasal tip
- Boxy nasal tip
- Pinched nasal tip
Tip rhinoplasty therefore entails modifying the size and shape of the underlying cartilages. These cartilages are known as the lower lateral cartilages and make up the nasal domes. These cartilages can be trimmed to reduce their size and prominence. This can have the effect of producing a finer and more refined nasal tip. This can also have the effect of lifting the tip up slightly, which can have a good aesthetic effect in individuals with a ‘plunging tip’ (a nasal tip that drops, or is accentuated with smiling), or in women who desire a slightly upturned nasal tip.
Other procedures that are performed to achieve nasal tip definition and refinement include the placement of specific ‘tip defining’ sutures. The sutures can be placed within (intradomal) the lower lateral cartilages to create and sharper and more refined nasal tip. Similarly, sutures, can be placed between (interdomal) the cartilages to narrow the nasal tip.

Total rhinoplasty entails not only addressing the nasal tip, but the entire nasal structure.The various parts of the nose that are frequently addressed during a total rhinoplasty include:
- Tip rhinoplasty to refine the nasal tip
- Repositioning of the nasal tip
- Addressing a prominent nasal bump or nasal hump
- Narrowing the bridge of the nose
- Using cartilage grafts to ensure adequate nasal support for the new shape
- Addressing the nasal septum (septoplasty)
Nasal tip repositioning
The nasal tip position is characteristically different in men and women. Determining whether a nasal tip is too low or high is often assessed by the columella-labial angle. This is the angle that is formed between the lowest part of the nose and the upper lip. Typically, in men is 90 degrees. In women, the ideal angle is typically described closer to 95 degrees.ie a slightly more upturned nasal tip is often desirable in women.
There are various manoeuvres that can be undertaken to adjust tip position (tip height). These include:
- Trimming the lower lateral cartilages (as shown in red)
- Suturing the nasal domes up to the nasal bridge cartilage
- Reducing the columella

Nasal hump correction
The top or front surface of the nose is referred to as the nasal dorsum. This more often referred to as the nasal bridge. The nasal bridge can exhibit prominences known as a nasal hump (or dorsal hump). This type of nasal prominence can lead to a convex profile to the nose. Nasal humps may have formed as part of normal nasal development or may have arisen following nasal trauma.
The upper part of the nasal hump is typically made up of bone, whilst the lower part is cartilage. Reducing a nasal hump therefore frequently entails reducing the prominent bone and cartilage. Cartilage being softer, can be trimmed or shaved off with a surgical scalpel or scissors. The bony component however requires removal with a surgical chisel or bur. Fine-tuning of the bone surface to remove any small irregularities can then be undertaken with surgical rasps.
Slightly different aesthetic ideals in nasal profile are typically described in men and women. The goal is to generally create a straight nasal profile in males, whilst in females, a subtle concavity is often desired to create a more petite, slightly upturned nose. Again, these changes should not be exaggerated in females, unless of course a more ‘ski jump’ style nose is specifically requested. Ethic variation and preferences also need to be carefully considered and discussed prior to surgery to ensure that the right nasal profile is achieved.


Depending on the degree of hump reduction that is undertaken, other manoeuvres may be required to achieve the optimal nasal profile and nasal shape. With significant dorsal hump reductions, a phenomenon known as ‘open roof’ may develop.
The way to think of this, is to consider the nose as a pyramid, consisting of two side pillars and a central pillar. The two side pillars are the opposing nasal bones and the central pillar is the nasal septum. When the top of the pyramid (dorsal hump) is trimmed off, the 3 pillars will no longer meet at the top i.e. a gap is created between the 3 pillars at the top. This is known as an open roof deformity, and if left, will need to visible depressions in the overlying skin. The open roof therefore needs to be corrected and this is performed by way bridging the gap (between the upper ends of the pillars) with cartilage, and or by bringing the nasal bones (two side pillars) inwards.
Bridging the gap with cartilage can be done by folding any existing excess cartilage inwards and these are then known as dorsal spreader flaps. Alternatively, the gaps can be filled by inserting thin struts of cartilage, and these are known as dorsal spreader grafts. These struts of cartilage can be obtained from the nasal septum, which is another area of the nose where spare cartilage can be obtained.
As one can see, changing one part of the nose during rhinoplasty often necessitates other procedures to be performed to ensure an ideal result is achieved. This is why rhinoplasty surgery is considered one of the most technically challenging aesthetic procedures in plastic surgery. It is important to ensure that your surgeon not only has an aesthetic eye, but a good understanding of nasal anatomy and the various factors that interplay during rhinoplasty surgery.
Narrowing the nose
Reducing the width of the nose can be achieved by moving the nasal bones inwards. Small osteotomies (small breaks in the bone) along the desired path, and in a controlled manner are made along each nasal bone. The osteotomies are commonly performed in a “low to high” or “low to low” manner depending on the desired repositioning for the bones.
Once the osteotomies are performed, this then allows the bones to be shifted inwards to the desired nasal width. When the procedure is performed, it is important that the direction of the osteotomies are done in a very controlled manner to avoid untoward complications or multiple levels of breaks. This minimises the chance of also being left with any visible or palpable bony irregularities.

Bringing the nasal bones inwards has the effect of narrowing the bridge of the nose. In selected cases it is also desirable to narrow the width of the nostrils.
The latter entails undertaking what is known as sill reduction or alar base reduction. These manoeuvres entail removing a strip of tissue from the nostrils, enabling them to be narrowed. The incisions are positioned along the creases around the nostrils, so that the resulting scar is typically very well concealed.
Do I need nasal Cartilage grafts?
When undertaking rhinoplasty, it is almost a routine part of my practice to place structural cartilage grafts with in the nose. This has the advantage of ensuring adequate support is provided to the new nasal shape. This plays an important role in maintaining nasal shape, particularly tip projection (which tends to drop with age) in the long term. Cartilage grafts may also be required to optimise the nasal airway and help correct any pre-existing nasal obstruction.

Cartilage grafts can also be trimmed, shaped, and placed in the nasal tip region to augment tip shape. These are known as onlay grafts. In individuals with short or stubby noses, onlay grafts can have the benefit of increasing nasal tip projection and creating a more refined nasal tip.

Reducing a prominent nose
Prominent noses may be because of increased nasal projection, increased nasal length, and or an increased nasal bridge. It is important to keep in mind that no matter what is done to reduce a prominent nose, consideration needs to be given to the rest of the facial dimensions to ensure that the nose remains proportionate. For example, in someone with a prominent nose, an excessive reduction in nasal size, can end up making the chin look disproportionately larger.
Nasal projection
Nasal projection refers to how far forward the nasal tip projects forward from the face.
How can one reduce nasal projection?
The amount of tip projection that one sees, correlates to the length of the cartilages that form the nasal tip. The cartilage that form the tip are referred to as domal cartilages. The domal cartilages can be further broken down into 3 sections, namely medial, middle and lateral crus.
Tip projection can be adjusted by adjusting the one or more of these crus. Adjusting the crus usually entails dividing the cartilage and then sliding one cartilage over the other. This overlapping of cartilage allows the length of the cartilage (and hence nasal tip projection) to shorten. The overlapping also ensures that the cartilage remains sturdy, whilst also minimising the chance of a kink forming at the site of cartilage division.

Depending on whether the middle or lateral crus (or both) are shortened, the tip projection can not only be reduced, but rotated up or down. It is therefore important that your surgeon has good experience and understanding of the way cartilage modification procedures impact on nasal shape and tip position.
How can one increase nasal projection?
In individuals with reduced nasal tip projection, nasal length can be increase using cartilage suture techniques and or cartilage graft procedures.
Nasal tip projection can be reduced in certain ethnic groups (Asian or African descent), following trauma, or as part of ones’ genetic makeup.
Refining the nasal tip and undertaking both intradomal (with in domes) and interdomal (between each dome) cartilage sutures can increase nasal tip projection. Where significant increase in nasal projection is required, typically cartilage grafts are required. This may take the form of onlay cartilage grafts, where by small pieces of cartilage (sourced from the septum or ear) are shaped and sutured onto the existing nasal cartilages ins layered fashion.

Where maximal increases in nasal projection are required, a rib graft rhinoplasty (see following section) may be undertaken. Silicone implants or their equivalent are alternative options to achieving increased nasal projection. One of the limiting factors that one must keep in mind, is the quality and adequacy of the skin available, to accommodate the increased projection.
Rhinoplasty FAQs
WHAT IS A SEPTOPLASTY?
WHAT IS REVISION RHINOPLASTY?
WHAT CAN I EXPECT AFTER SURGERY?
WHAT IS THE RECOVERY?
WHAT DOES MY AFTERCARE INVOLVE?
WHEN CAN I SEE THE FINAL RESULTS?
HOW MUCH DOES RHINOPLASTY COST?
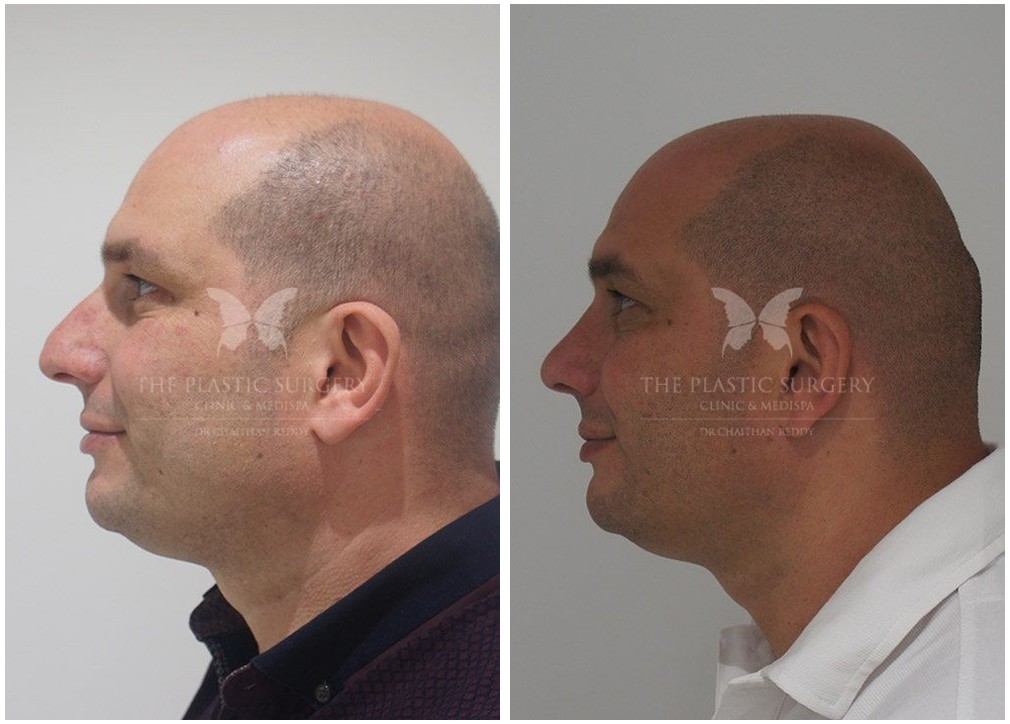
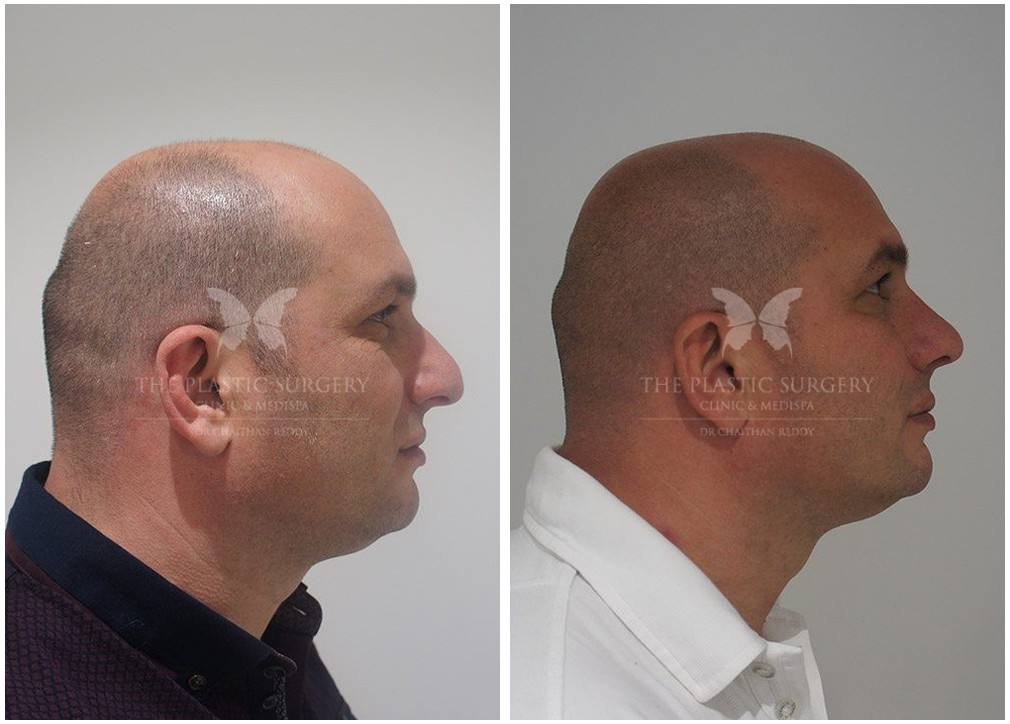
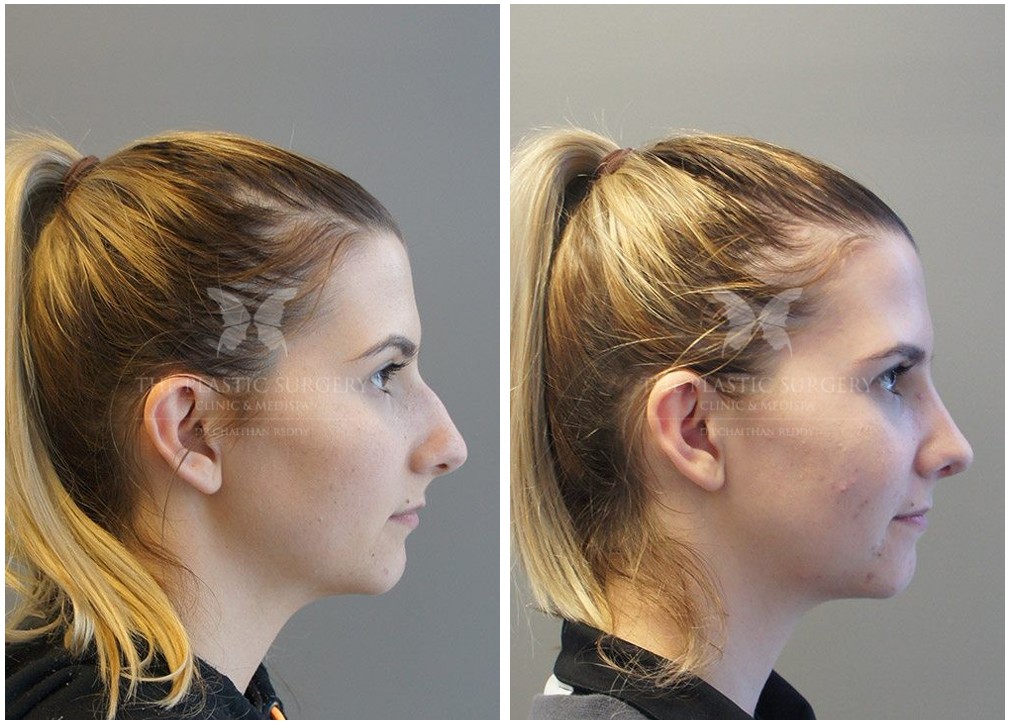
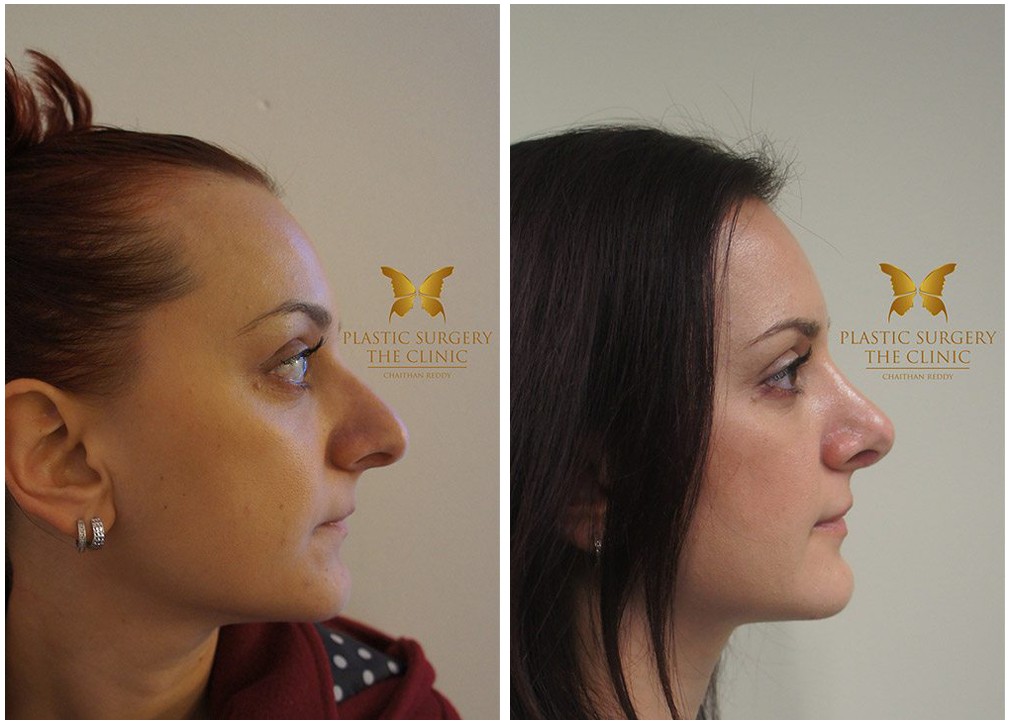
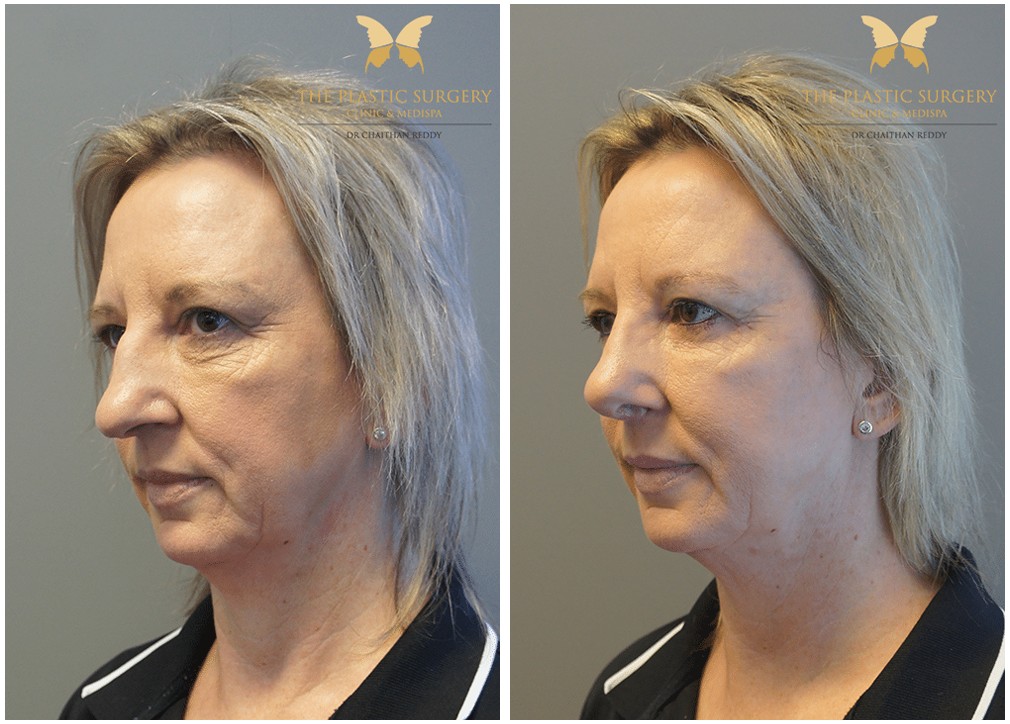
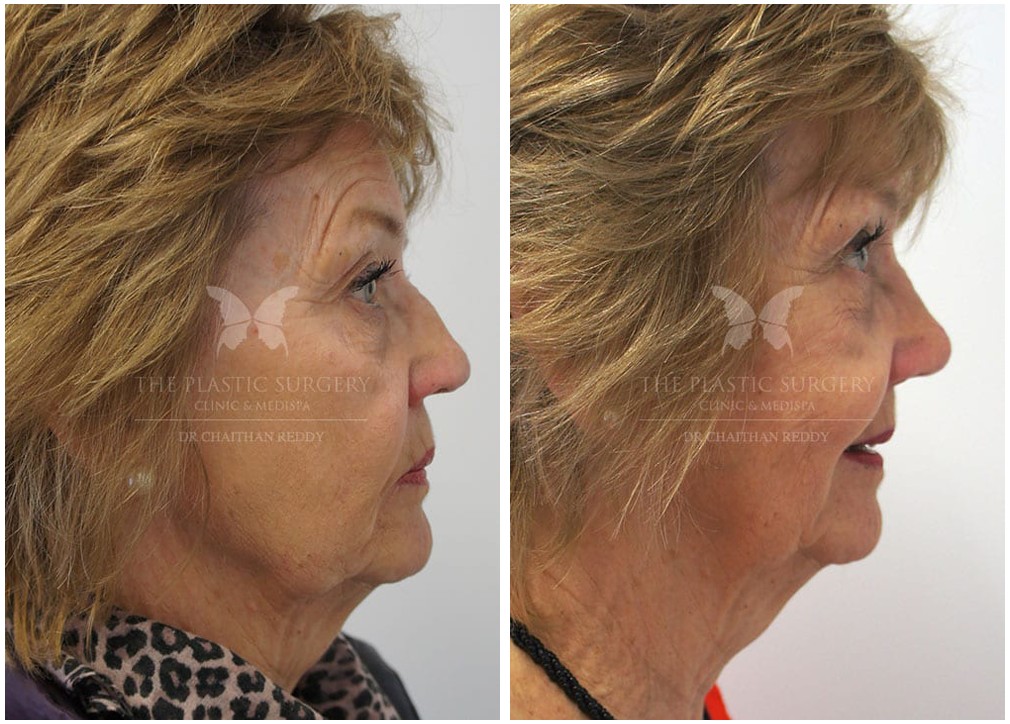
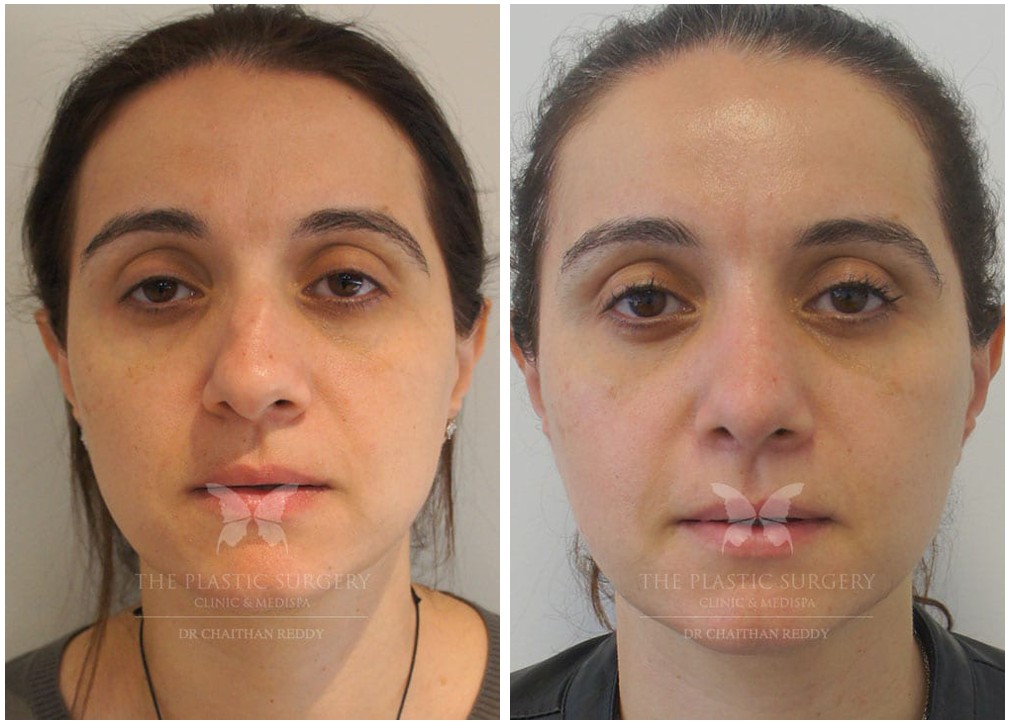
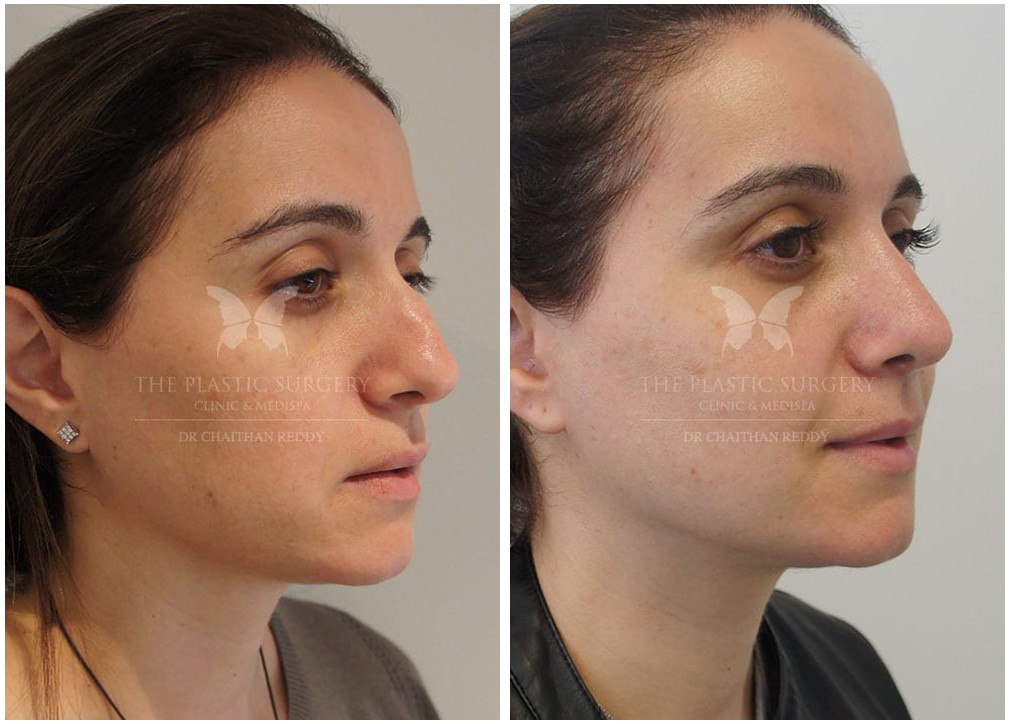
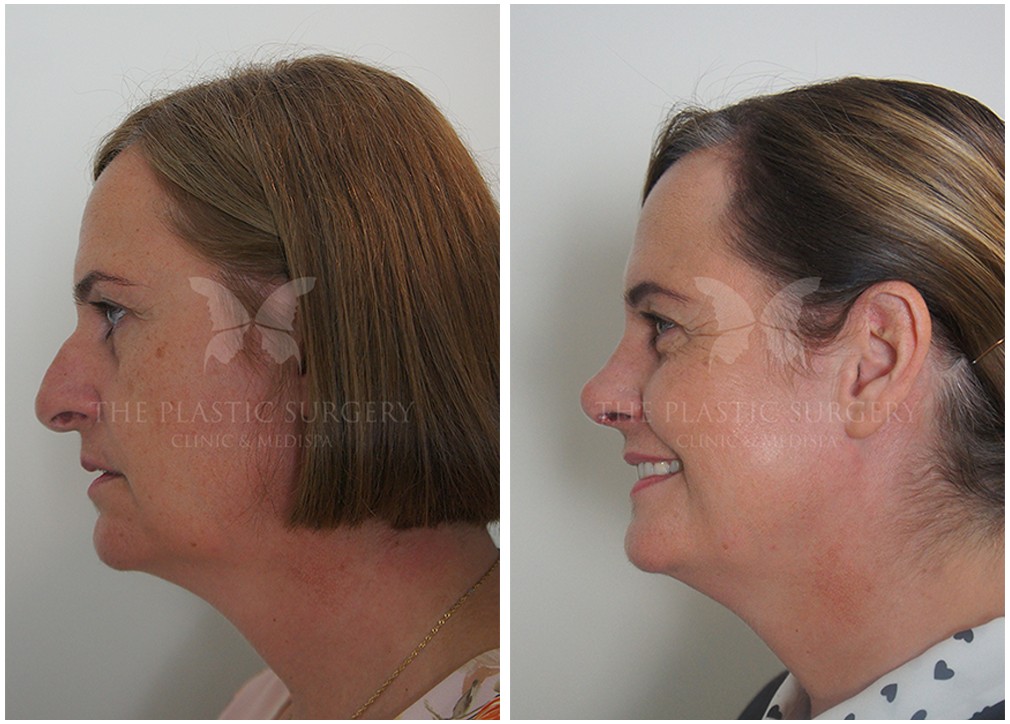
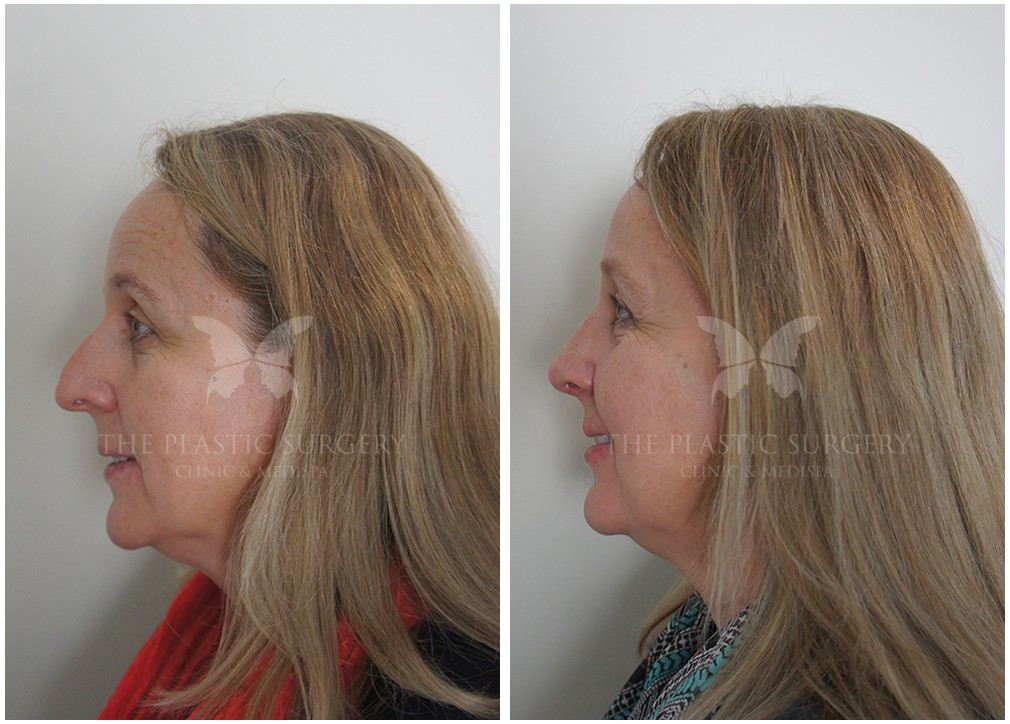
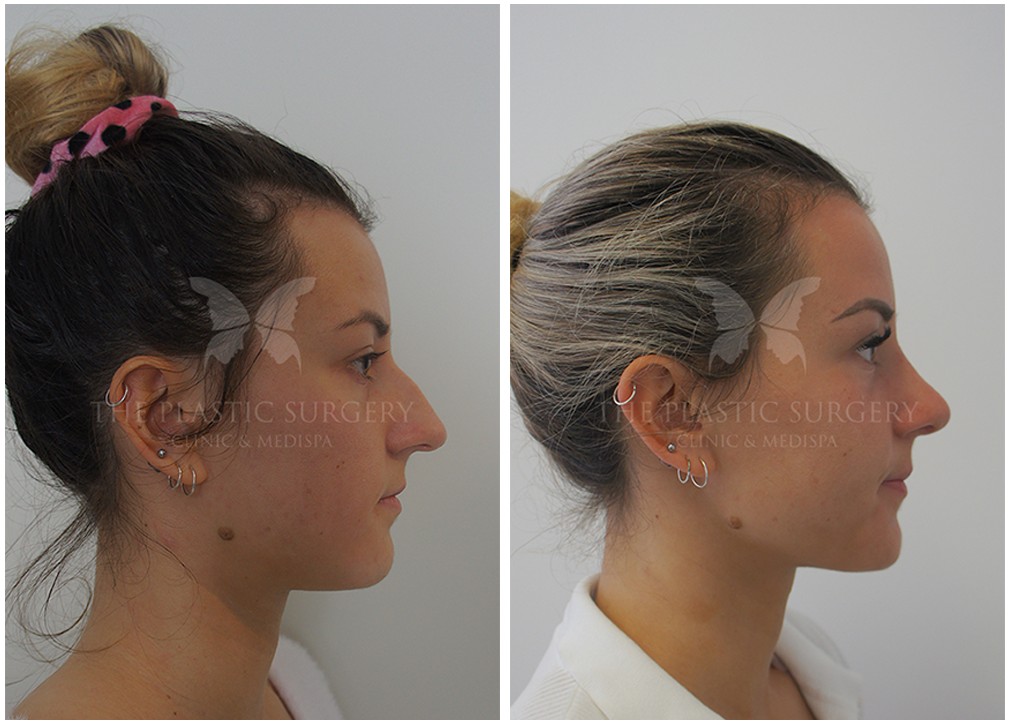
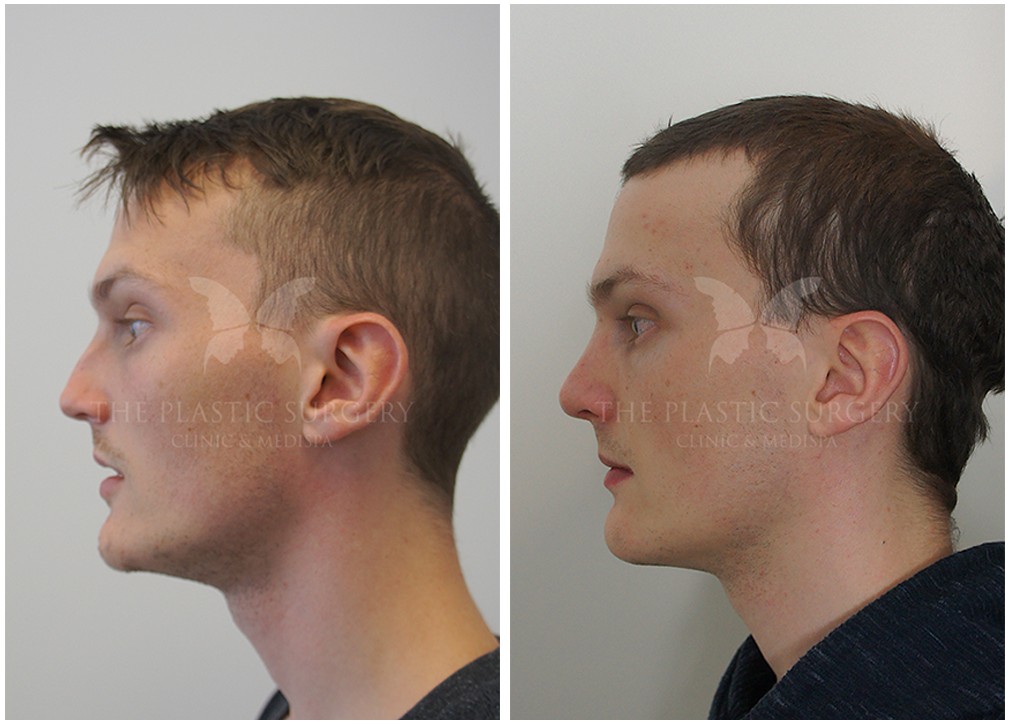
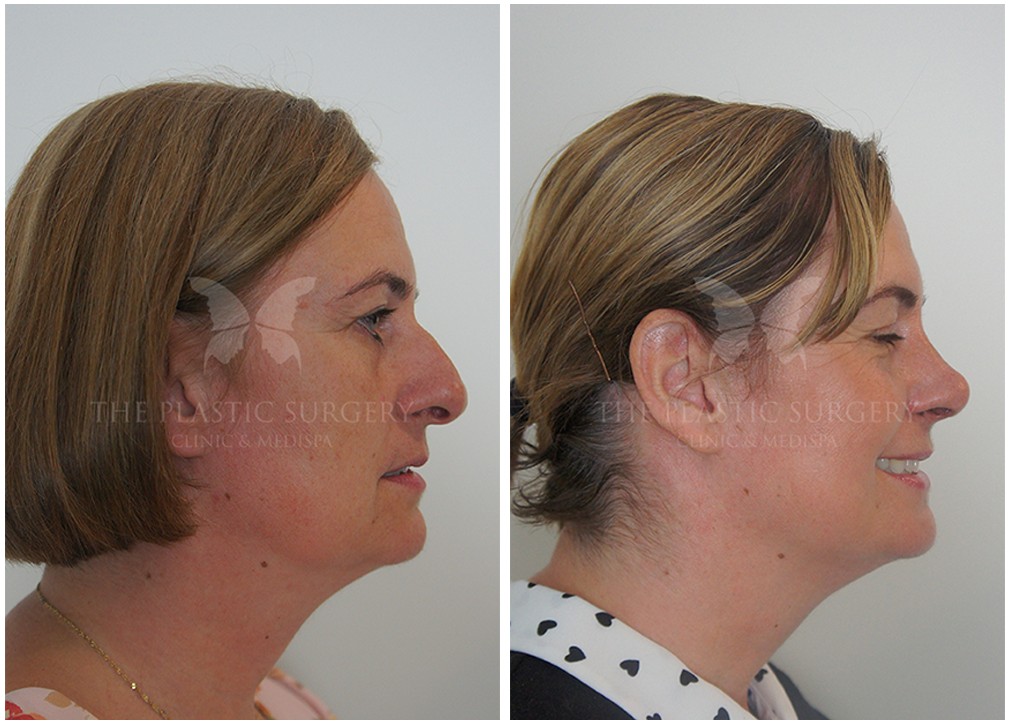
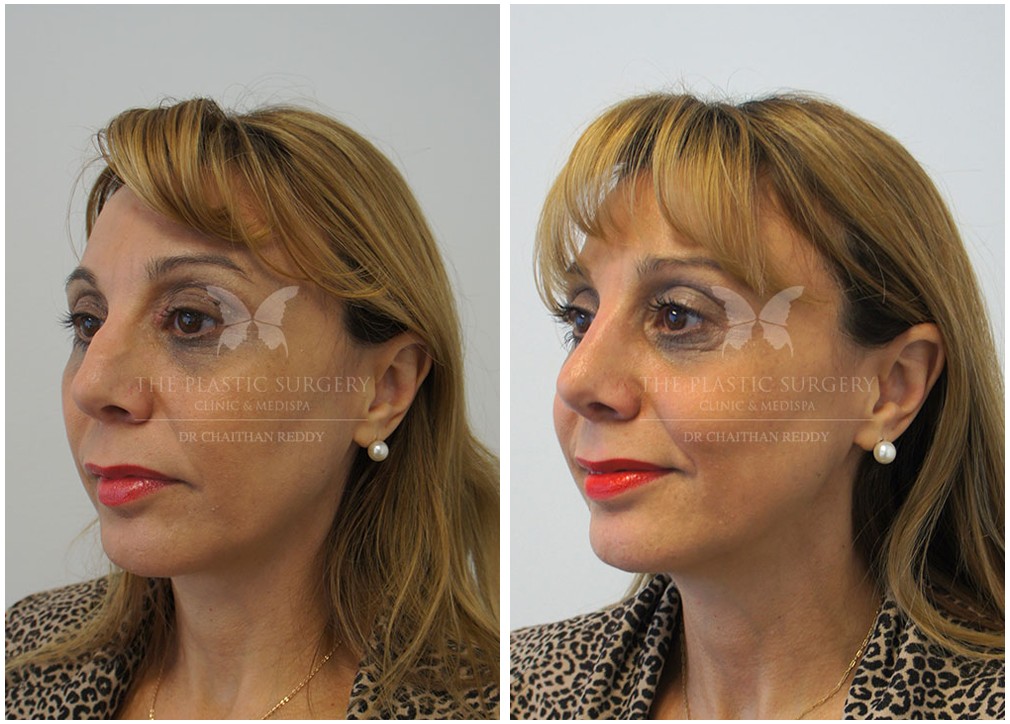
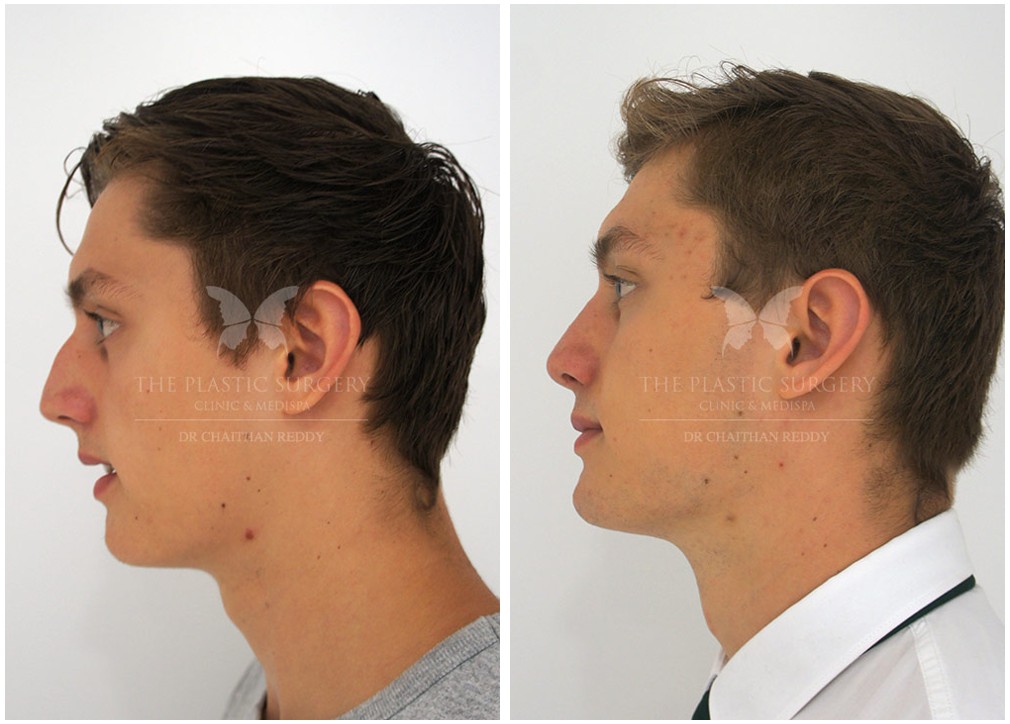
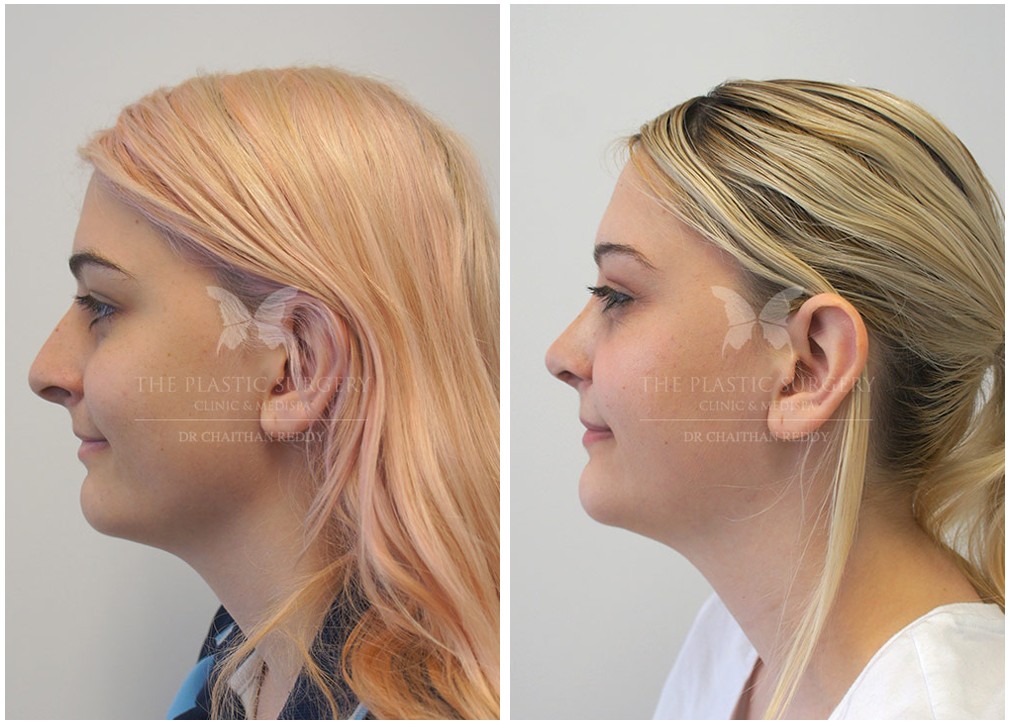
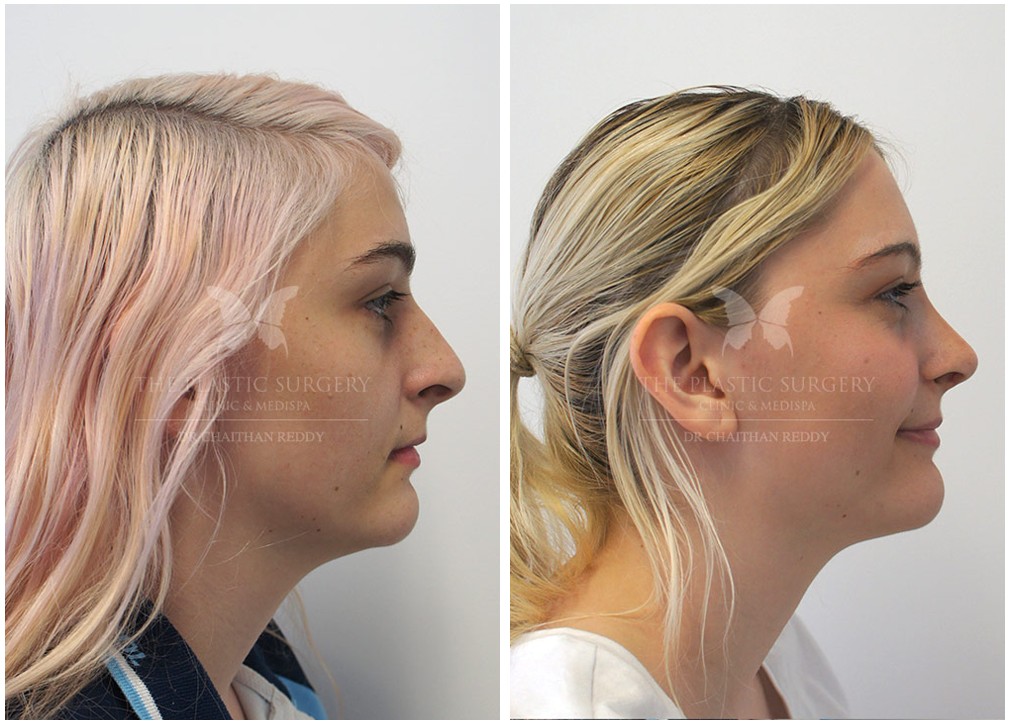
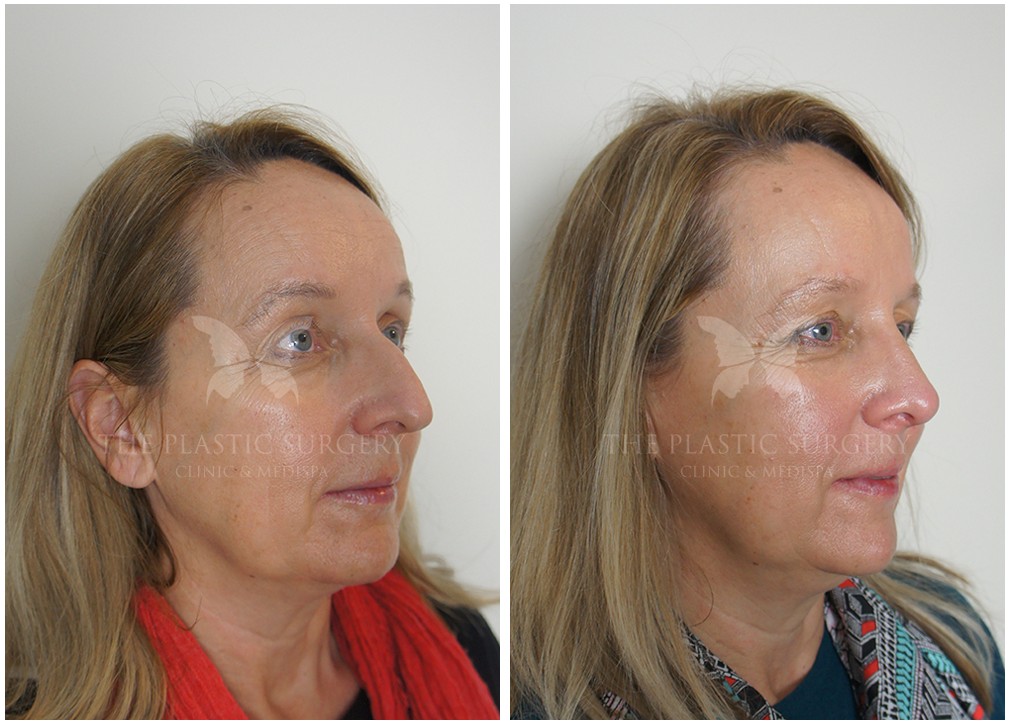
Rhinoplasty Before And Afters
Nose Surgery in Sydney
If you are dissatisfied with the appearance of your nose, or if you have breathing difficulties that would improve through surgical correction of your nasal anatomy, then arranging a rhinoplasty consultation with Dr Chaithan Reddy may be ideal for you.
Every patient is unique and results may vary. Surgery and all health regulated services carry risks which need to be discussed with your doctor to ensure you are fully informed and realistic outcomes have been explained.