Dr Reddy is a proud member of the following associations:


There are a number of surgical procedures that fall within the realm of Facial feminisation surgery. Such procedures include: hairline lowering, forehead reshaping, rhinoplasty, midface procedures, and lower jaw reshaping procedures. Depending upon one’s face shape, one or more of these procedures may be undertaken to achieve facial feminisation.
Dr Reddy’s expertise in Facial Feminisation Surgery
Dr Chaithan Reddy is a highly trained Plastic & Reconstructive Surgeon with over 15 years of clinical experience in the field. He has also trained in craniofacial procedures. Having also graduated with a Bachelor of Dental Surgery and being one of only a handful of Plastic & Reconstructive Surgeons with dual qualifications, he holds additional experience in Oral & Maxillofacial Surgery, allowing him to specialise in jawline procedures.
He is one of only a handful of FFS surgeons that offers the gamut of facial feminisation procedures, including complex Type 3 forehead reconstructions, hairline restoration, rhinoplasty, and lower jaw surgery. Having also completed a Master in Surgery focussing on Microsurgery, he is well versed in precise, technically challenging and complex procedures.
Well regarded by his peers and known for his technical expertise, he takes pride in his work and caring approach to his patients. He has authored multiple publications and has presented nationally, and internationally. He presented at the Australian Society of Aesthetic Plastic Surgeons (ASAPS) meeting in 2023 to a national and international audience on his techniques and approaches to facial feminisation surgery. Dr Reddy has since been requested back again as an invited speaker on Facial feminisation Surgery.
Dr Reddy has vast experience in facial feminisation surgery and is always directly involved in each patient’s perioperative care.
Pre-operative consultations are in person. Interstate and international patients can elect to have a telehealth consultation in the first instance if preferred. Post-operative reviews are undertaken in person regularly by Dr Reddy and are advised for at least 12 months following your surgery. Travelling patients can elect to have some of their post-operative reviews via telehealth if preferred.
Dr Reddy undertakes all aspects of facial feminisation surgery. He has been featured on Channel 10 as a surgeon with expertise in Facial Feminisation Surgery. Once you have decided to see Dr Reddy, a comprehensive one-hour discussion is undertaken at your first consultation, and a treatment plan is proposed. A second consultation is also required to ensure you understand the surgical plan and recovery process. Additionally, Dr Reddy routinely uses 3D image simulation to assist his surgical planning and provide you with a visual indication of the expected results.
In achieving such results, it is important that a comprehensive and dedicated team of medical providers are involved in the facial feminisation. journey. While Dr Reddy will be your facial feminisation surgeon, several other members form an important part of your care.
| As featured on Channel |
Meet the other members of our facial feminisation team
Assoc. Prof Faruque Riffat (ENT SURGEON)
Dr Sanjay Sharma (Anaesthetist)
Dr Daniel Kwok (Anaesthetist)
Dr Ernest Wong (Anaesthetist) MBBS FANZCA
Susan Garrett (Aesthetic Nurse)
Rebekah Langford (Registered Nurse)
Julianne Kim (FFS Patient Coordinator)
WHAT constitutes facial feminisation Surgery?
Facial Feminization Surgery (FFS) is a transformative medical procedure designed to alter and feminize facial features, providing a sense of congruence between a person’s gender identity and their outward appearance. The surgery plays a crucial role in the broader context of gender-affirming care, catering specifically to transgender women and gender-nonconforming individuals seeking to align their appearance with their true identity. The procedure can have a life-changing impact, contributing to improved self-esteem, mental health, and overall quality of life for those who undergo it.
Facial Feminization Surgery is a comprehensive set of procedures that address various facial features commonly associated with masculinity. The specific techniques and combination of procedures performed may vary based on each individual’s unique facial anatomy and desired outcomes. The surgery can involve reshaping the forehead, hairline, eyebrows, nose, cheekbones, lips, jawline, and chin. The procedures can also be considered reconstructive in nature with resulting therapeutic and cosmetic outcomes.
Key Procedures Involved in FFS include:
- 1. Forehead Contouring: The surgery reduces the prominence of the brow ridge creating a softer and more feminine forehead.
- 2. Rhinoplasty: Nose reshaping can be performed to achieve a more delicate and feminine nasal appearance.
- 3. Brow Lift: By lifting and shaping the eyebrows, FFS aims to create a more feminine brow arch.
- 4. Cheek Augmentation: Adding volume to the cheeks can create a more rounded and youthful appearance.
- 5. Lip Augmentation and or lip lift: The procedure elevates the upper lip, increases dental show and enhances lip fullness and shape to achieve a softer and more feminine pout.
- 6. Jaw and Chin Contouring: By reducing the size and squareness of the jaw and reshaping the chin, FFS can achieve a more delicate and feminine facial contour.
CONSIDERATIONS IN FACIAL FEMINISATION SURGERY
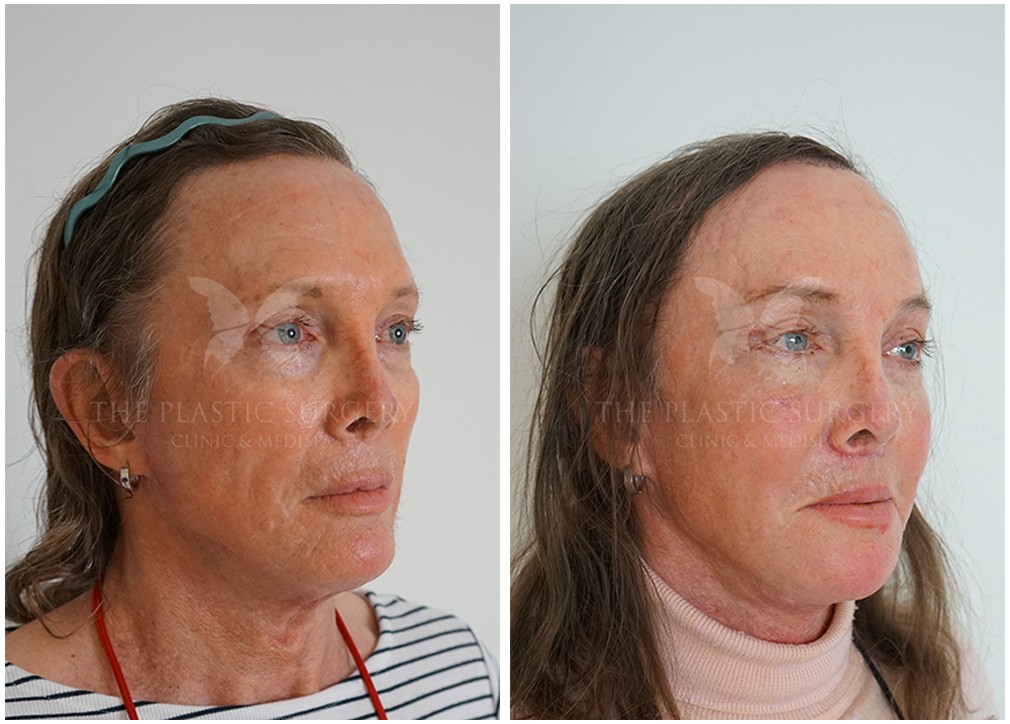
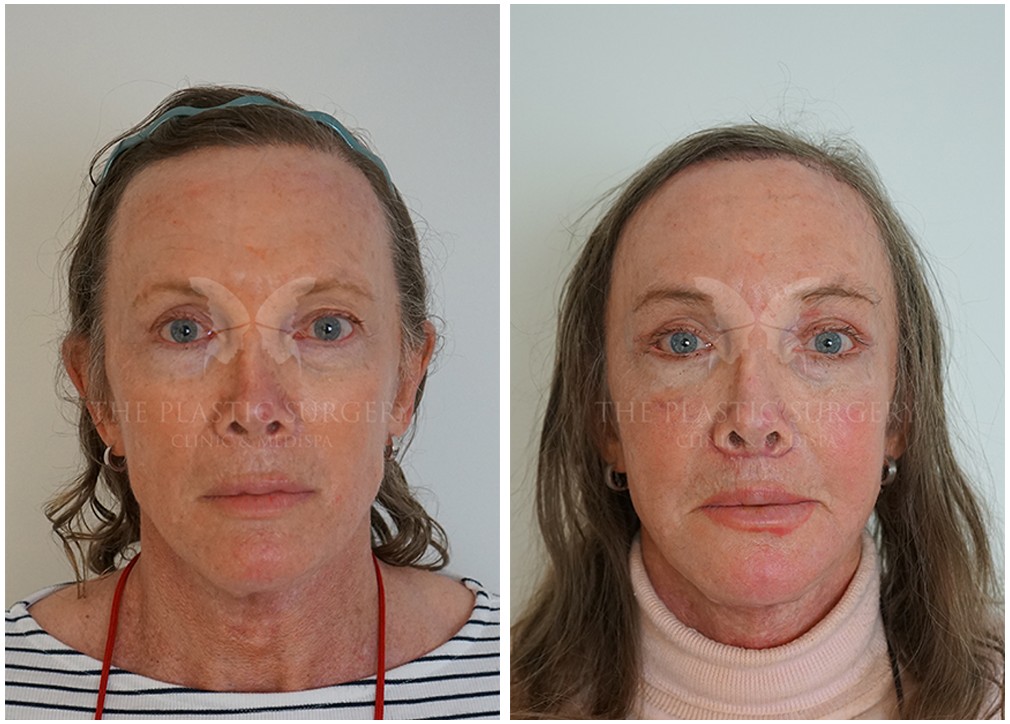
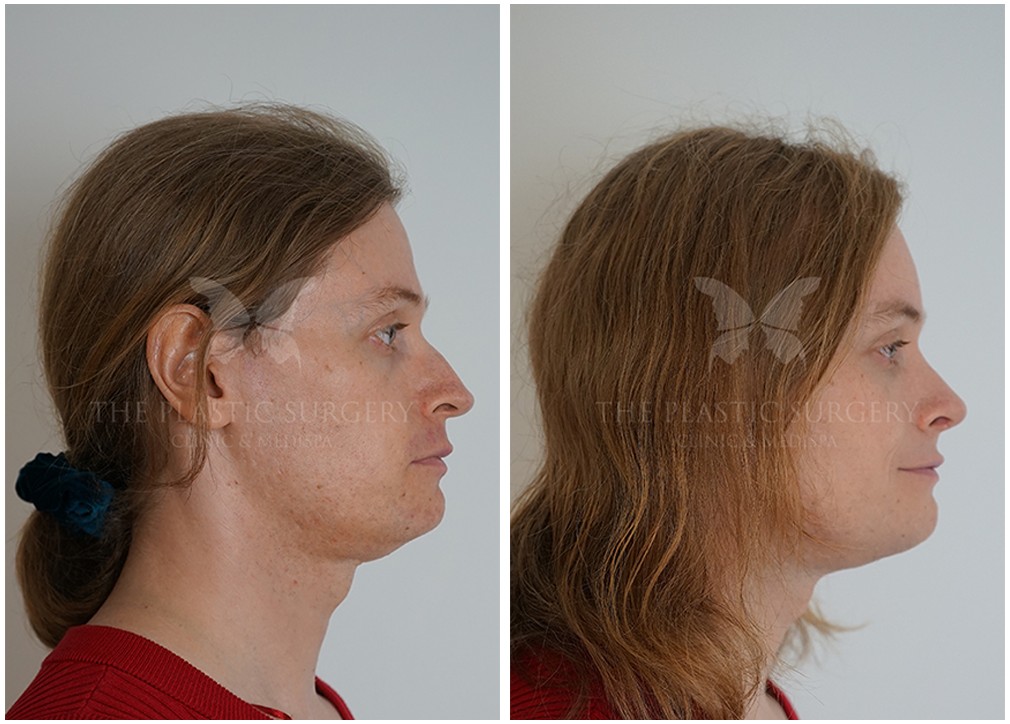
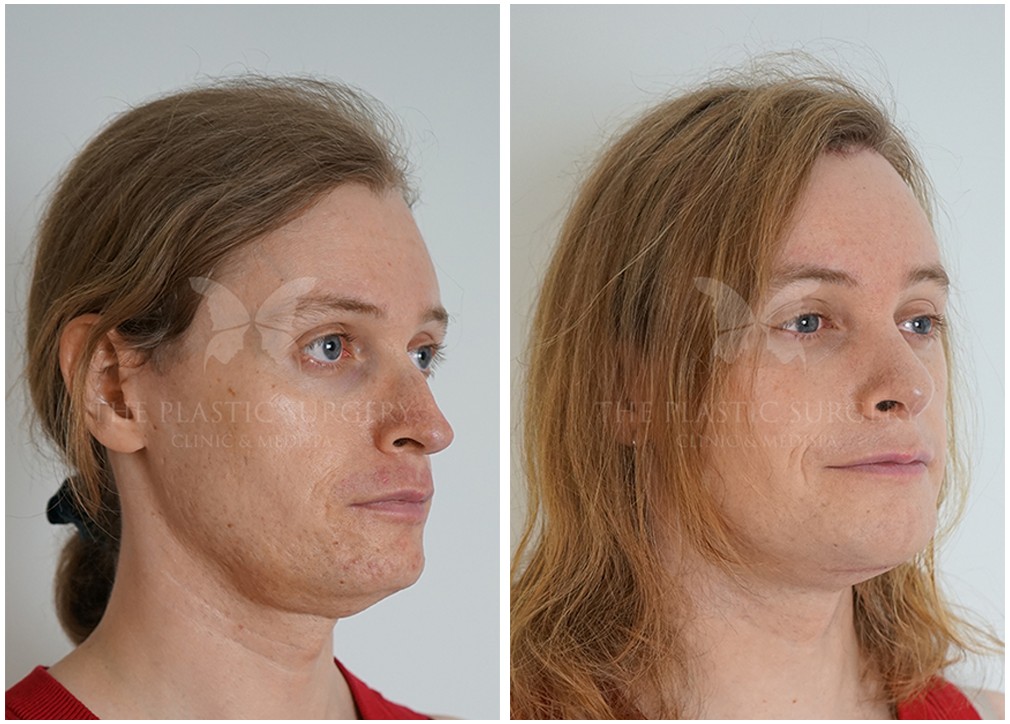
Facial Feminization Surgery has positively impacted the lives of countless transgender women and gender-nonconforming individuals. By providing the opportunity to align external appearance with internal identity, FFS plays a vital role in gender affirmation and empowerment. With ongoing advances in surgical techniques and increased awareness, FFS continues to be a transformative and life-affirming option for those seeking to embrace their authentic selves.
When is the right time to have surgery?
There is no right answer to this question. The answer will often depend on various individual factors. The primary factor will largely be dictated by when you feel ready to physically feminise your face to bring harmony to your gender identity. The purpose of the surgery is to assist you in achieving an outward appearance that is in keeping with this. It is important to note that Facial feminisation can also be performed to feminise the face irrespective of one’s gender identity. An important consideration is the duration of hormone therapy. Hormone therapy can influnce fat distribution in the face in some individuals and it therefore may be important to assess the response to hormones over a 6-12 month period before undertaking midfacial and neck procedures. This consideration will have minimal if any relevance to forehead and nasal procedures.
Facial feminisation may be undertaken before or after potential sexual reassignment surgery (SRS). The decision about the sequence of surgery will often be a personal one based on an individual’s preference and what they feel will serve them most in achieving their desired gender identity. Some individuals may feel that undertaking SRS first will help them formalise their gender identity. Others may feel that changing their outward facial appearance with facial feminisation first will help them feel more accepted as a female in society.
Medical considerations in FFS
Requirements to undergo Facial Feminization Surgery (FFS) in Australia may vary depending on the specific surgeon or healthcare provider and the guidelines they follow. Please note that medical guidelines and criteria may also change over time. However, some general criteria that are typically considered for patients seeking FFS are as follows:
- 1. Generally, patients seeking FFS would have a diagnosis of gender dysphoria or have a confirmed gender identity different from the sex assigned at birth.
- 2. Psychological Evaluation: Patients may be required to undergo a psychological evaluation to assess their mental health, readiness for surgery, and expectations regarding the outcomes of FFS. The evaluation helps ensure that the individual is emotionally prepared for the procedure and has realistic expectations.
- 3. Age Requirement: The minimum age for undergoing FFS may vary depending on the surgeon or healthcare provider. Some may have age restrictions and require patients to be at least 18 years old before undergoing the procedure.
- 4. Hormone Therapy: Some surgeons may prefer patients to be on hormone therapy for a certain period of time before FFS. Hormone therapy helps to induce physical changes, such as fat redistribution and skin changes, which can enhance the effectiveness and natural appearance of the surgical outcomes.
- 5. Real-Life Experience: Some surgeons may require patients to undergo a real-life experience or a period of living as their identified gender before proceeding with FFS. This experience serves to confirm the patient’s commitment to their gender identity transition.
- 6. Medical Health Assessment: Patients will undergo a thorough medical assessment to ensure they are in good health and able to undergo surgery safely.
- 7. Informed Consent: Patients are required to provide informed consent, demonstrating that they understand the surgical procedures, potential risks, expected outcomes, and post-operative care requirements.
It is essential to research and choose a reputable surgeon who specializes in gender-affirming surgeries and has experience performing Facial Feminization Surgery. Each surgeon or healthcare provider may have their own specific criteria and guidelines, so it’s crucial to have a thorough consultation with the chosen surgeon to discuss personalized treatment plans.
Benefits of facial feminisation surgery
Research on the benefits of Facial Feminization Surgery (FFS) continues to grow, with studies focusing on various aspects of the procedure and its impact on transgender women and gender-nonconforming individuals. Here are some key areas of research and the potential benefits identified in studies:
- 1. Gender Dysphoria Reduction: Gender dysphoria refers to the distress experienced when there is a mismatch between one’s gender identity and physical appearance. FFS has been shown to significantly reduce gender dysphoria in transgender women. A study published in Plastic & Reconstructive Surg Glob Open Journal in 2023 found that FFS led to a substantial decrease in gender dysphoria and improved overall quality of life for the participants.
- 2. Psychological Well-being: Several studies have reported positive psychological outcomes following FFS. Research published in Annals of Surgery Journal, Plastic and Reconstructive Surgery Journal, and Facial Plastic Surgery & Aesthetic Medicine 2022 journals found that FFS was associated with improvements in self-esteem, body image, and satisfaction with facial appearance. Studies have also shown that patients reported increased psychological well-being and improved social functioning after FFS.
- 3. Quality of Life: FFS has been linked to a higher quality of life for transgender women. A studies published in Quality of Life Research in 2010 and Facial Plastic Surgery & Aesthetic Medicine in 2022 found that patients experienced significant improvements in social, emotional, and functional well-being after FFS. The procedure contributed to increased self-confidence and comfort in social situations, leading to a better overall quality of life.
- 4. Passing and Authenticity: “Passing” refers to a transgender individual being perceived and accepted as their gender identity by others. FFS can play a vital role in enhancing a person’s ability to pass as female, which is crucial for their safety and well-being. Several journal articles report that FFS was associated with a higher likelihood of passing and feeling authentic in social interactions. More recently, research published in the Journal of Craniofacial surgery in 2023 reported that transfeminine patients experienced improvements in satisfaction with facial appearance, and perceived gender.
- 5. Satisfaction with Surgical Outcomes: Overall, patients who undergo FFS tend to be satisfied with the surgical outcomes. A study published in the Journal Sexual and Relationship Therapy in 2019 and in the Journal of Plastic & Reconstructive Surgery in 2020 reported high satisfaction rates with FFS among transgender women, particularly concerning facial appearance and gender identity alignment.
- 6. Impact on Mental Health: FFS has been shown to have a positive impact on mental health outcomes for transgender women. Several studies, including data published in the Annals of Surgery in 2023 demonstrated a significant reduction in depression and anxiety symptoms following FFS.
It is important to note that while the research indicates many benefits of FFS, individual experiences and outcomes may vary. It is essential for patients to have realistic expectations, and have open communication with their surgical team to ensure the best possible results and psychosocial well-being.
How does Dr Reddy feminise the face?
In answering this question, the fundamental differences between male and female facial anatomical characteristics need to be understood. Anthropologic studies have clearly demonstrated key sex differences between the male and female facial skeleton. It is in understanding and addressing these sex differences that allows Dr Reddy to create a female appearance to the facial region. Whilst soft tissue characteristics such as the skin, hair growth, fatty tissue distribution, hairline and lips are important considerations, fundamental differences lie at a deeper level. We know from history and our study of human anatomy, that the male facial skeleton is typically larger and broader. Reducing both horizontal and vertical dimensions of the facial skeleton therefore play an important role in feminising the face. Once the underlying framework is addressed, the outer covering (soft tissues) so to speak can be addressed to optimise the final outcome.
Common skeletal differences between the male and female facial skeleton include:

- Browbone prominence typically seen in males
- Relatively increased height and shape of the eye socket in women
- Increased width to the lower jaw typically seen in males

- Prominence of the brow bone segment in males
- A deeper angle (NFr) between the forehead and nose in males
- Increase height to the lower jaw
- More acute lower jaw angle
Dr Reddy has extensive experience in surgery addressing both the soft tissues and bone structures associated with the facial region. He has undertaken thousands of procedures entailing these structures. By combining this experience with knowledge surrounding sexual differences in facial anatomy, he is able to achieve a feminised appearance to the facial region. The process commences with consultation involving an in-depth assessment of your desires and existing facial features and proportions. Clinical measurements combined with three-dimensional digital imaging allows for accurate assessment and documentation of your facial shape. Radiological investigations including x-rays and CT scan imaging is organised to further assess the facial skeleton. Based on this information, a clear detailed surgical plan is provided to you. The relevant procedures are further discussed in detail and an information pack pertaining to each specific procedure is provided to you. This will include information pertaining to your recovery and healing phases.
Do I need to have all the procedures at once?
There are multiple procedures that fall under the domain of facial feminisation. These include Hairline lowering, forehead reshaping, brow lift, rhinoplasty, cheek augmentation, lip lift and augmentation, jaw reduction, and facelift surgery. It is important to consider that all patients present differently and may only have certain masculine features that require correction. I.e. There is no requirement to have all procedures undertaken, or even if needed, there is no requirement to have the procedures undertaken at once. Following the consultation process, Dr Reddy will be able to advise you on what procedures may best benefit you in achieving a feminine face. Whilst Dr Reddy can undertake all relevant facial feminisation surgical procedures in the same setting, in some instances, it may be preferable to stage the surgery in the interest of patient safety, or in achieving the optimal result. Dr Reddy will discuss this with you during the consultation process.
What are the risks associated with surgery?
Like any surgical procedure, Facial Feminization Surgery carries potential risks and complications.
Risks can be classed as general risks associated with anaesthesia and surgery in general, and also specific risks associated with individual FFS procedures.
General risks include anaesthetic related complications, but these are rare. Other general risks that are very uncommon include infection, bleeding or healing related problems. Deep vein thrombosis (DVT) is a risk associated with any surgery, but the incidence is extremely low. It is important to discuss your hormone therapy regime with your treating doctor as this can be relevant to your DVT risk.
Specific risks can include prominent or visible scars, altered nerve function (numbness or altered sensation, weakness), sinus infection (Type 3 forehead reconstruction), palpable bone plate or screws.
Dr Reddy will discuss these in detail with you during the consultation process.
Choosing a highly experienced and qualified surgeon significantly reduces the likelihood of complications.
It is crucial for individuals considering FFS to have a clear understanding of the surgical process and potential outcomes. A candid discussion with the surgeon and other transgender women can provide valuable insights and support during the decision-making process.
What are the costs associated with surgery?
There is no one specific cost for facial feminisation procedures. Every individual presents with different feminisation surgery requirements. Similarly, not all facial feminisation procedures may be required to achieve the desired endpoint. Following the consultation process an individualised treatment plan is put together and a fee schedule based on your individual requirements is provided to you. This will provide you with accurate idea of all the relevant costs. The costs to consider include surgical fees, hospital related costs, anaesthetic fees and assistant fees. Interstate and international patients need to also consider travel and accommodation costs. Your surgical fees will cover the cost of your post-surgical care and reviews.
Are the changes permanent?
The changes are typically considered irreversible for certain facial feminisation procedures. It is therefore important that you have considered this carefully in the decision making process.
What are the post operative recovery and outcomes like?
Recovery times can vary based on the extent of the procedures performed. Swelling and bruising are common after FFS. Bruising typically resolves in a two week time frame. Swelling can take longer and this subsides over the course of several weeks, although may not be that obvious even after two weeks. The pain is typically not severe and is often well controlled with a combination of simple pain medications, and also stronger pain medications as required. These are typically provided prior to discharge from hospital.
The duration of your hospital stay will ultimately depend upon the type and number of FFS procedures that are being undertaken. The hospital stay typically ranges from 1 day to 3 days.
Depending upon the procedures being undertaken, one may need to also wear a compression garment. It is important that the procedure specific post-operative care instructions are followed to ensure proper healing. Dr Reddy will also go through this with you in the post-operative period.
Dr Reddy recommends having a support person with you during the first week after surgery. Whilst you will be in a position to attend to your self-care needs, a support person can be helpful in attending to other essential needs during the initial post-operative period. They can also assist you emotionally during this initial recovery period.
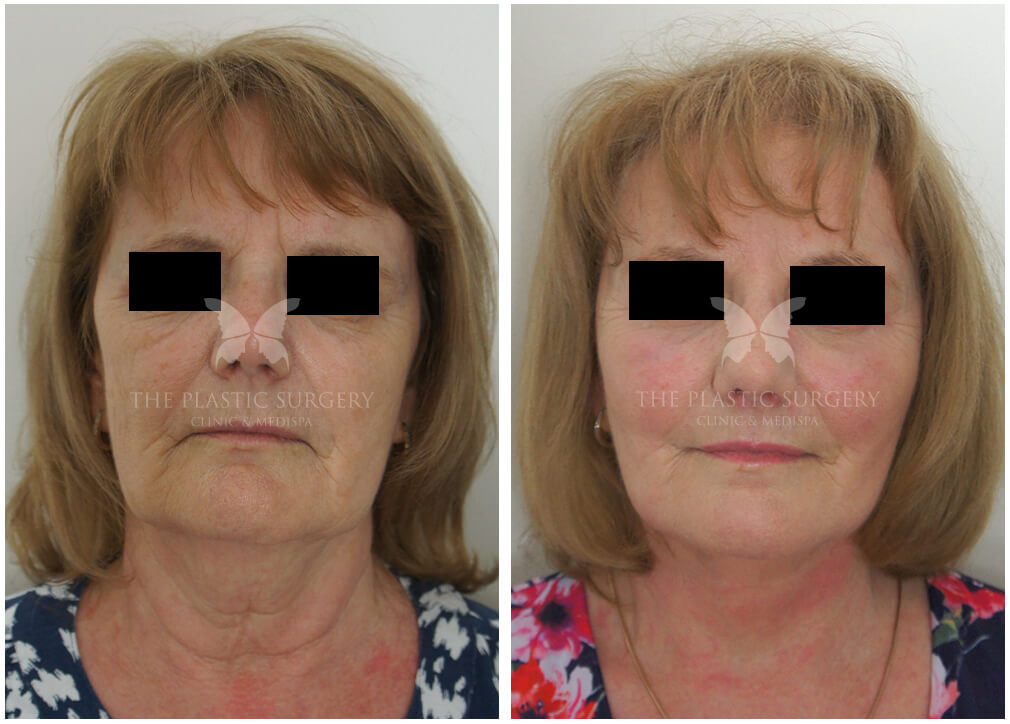
Following the initial post-operative recovery period, the results of Facial Feminization Surgery are often profound and life-changing. Many patients report feeling more confident, empowered, and aligned with their true identity. FFS can significantly contribute to improved mental health, reduced gender dysphoria, and a greater sense of self-acceptance.
Choosing the right surgeon?
When embarking on the journey of facial feminisation, this can entail a big commitment emotionally, psychologically, and financially. It is important therefore that you feel completely at ease with the surgeon that you choose to proceed with and entrust. Whilst a trusting doctor patient relationship is fundamental to the entire process, it is equally important to have a surgeon that is trained and experienced in such procedures. It is also important to have a surgeon with an excellent safety profile. Dr Reddy has extensive knowledge and experience in facial feminisation procedures. He has received training in dental surgery, maxillofacial procedures and Plastic & Reconstructive surgery, all essential components of facial feminisation surgery.
FACIAL FEMINISATION PROCEDURES
Before considering these procedures, one must understand the differences between a masculine and feminine face. A good way to think about this is to consider the face in facial thirds:
- (I) upper third, spanning from hairline to brow
- (ii) mid-third, spanning from brow to bottom of the nose
- (Iii) lower third, spanning from the bottom of the nose to the chin
For each of these facial thirds, various distinguishing features reflect male vs female characteristics. There are certain aesthetic ideals that one aims to approach in transforming from a male to a female face, and these are outlined below.
Forehead Reduction in Facial Feminisation Surgery
In the upper third of the face, the hairline, forehead shape and brow all need to be considered as part of one’s assessment during facial feminisation surgery. There are certain male vs female aesthetic ideals that need to be approached to achieve an optimal result. This, therefore, requires a good understanding of the sex differences that occur in the upper facial region.
When viewed from side-on, a male forehead tends to have a more prominent brow region. This is because the forehead bone situated under both brows tends to be more prominent in males. These sex differences in forehead contour and brow prominence are highlighted in the image below. The blue markings reflecting a softer and flatter brow bone contour, along with a more open orbital rim classically seen in a female facial skeleton, as opposed to the red markings depicting the more characteristic features of a male facial skeleton.

Facial Feminisation can therefore entail surgery to reduce or conceal the prominence of one’s brow bone region. Small prominences can be addressed by shaving down the underlying bone. Larger prominences entail reshaping the forehead bone in the brow region. Dr Reddy can do this by repositioning pieces of the forehead bone or by using bone substitutes to conceal the prominent area.
Forehead reduction and forehead reconstruction procedures are undertaken in hospital and under general anaesthesia. Accessing the bone typically entails an incision on the scalp. The incision location can vary depending upon whether a concurrent brow lift procedure or hairline lowering procedure is undertaken.
There are three main types of forehead reduction procedures. Type I procedures typically entail shaving down the prominent section of bone. The extent of this will depend on the thickness of the bone in this region and the size of the frontal sinus. If the bone overlying the frontal sinus is very thin, then a type I reduction is generally unsuitable for achieving the desired amount of correction. The outer portion of the bony rim of the eye socket can also be shaved down to correct prominence at the outer aspect of the brow.
A type II procedure may be undertaken, entailing bone reduction and augmentation of the area above the reduction site. This can also achieve the desired result of a smoothly contoured forehead. In cases where there is significant brow bone prominence, a type III procedure or forehead reconstruction is indicated. This entails removing a portion of the outer skull bone segment in this region and resetting the bone segment further back. This will achieve definitive correction in such cases of advanced brow bone prominence. The risks associated with each type of forehead procedure will increase according to the complexity of the procedure. Dr Reddy will discuss this in detail at the time of consultation.
The decision to proceed with a specific type of forehead reconstruction is largely dictated by the underlying anatomy and also the final forehead contour desired.
Significant brow bone prominence that is either noted by the patient or at the time of clinical assessment usually requires a type 3 forehead reconstruction. Facial feminisation of the upper third of the face commonly entails reducing this prominence in order to achieve a softer and less acute nasofrontal transition. This is referred to as the nasofrontal angle and typically ranges from 130 to 140 degrees. In females, the ideal nasofrontal angle should be ideally 135 to 140 degrees. In males, the nasofrontal angle is typically more acute based on anatomical and arthrometric studies.
The manner in which the desired contour and nasofrontal angle is achieved is dictated by the anatomy in this region. This pertains to the relationship between the thickness of the frontal bone and the size of the underlying frontal sinus. The frontal bone can vary in thickness and ranges from 1 to 10mm. In individuals with thick frontal bone, a type 2 forehead recontouring procedure may be adequate to achieve the desired result.
In individuals where the section of frontal bone that is situated in front of the frontal sinus is very thin, there is very little bone reduction that can be achieved with a shave procedure and a type 3 or 4 forehead reconstruction is required.
This entails repositioning of the prominent section of the frontal bone. CT scan and or cephalogram assessment is undertaken by Dr Reddy to assess the thickness of the bone and determine what procedure is best undertaken for each individual facial feminisation procedure.
Dr Reddy prides himself on careful and rigorous planning in forehead reduction procedures. Not only is a decision made on the type of forehead reconstruction procedure required, but the exact amount of bone to be reduced and repositioned is calculated in millimetres. This helps ensure that your final result matches the preoperative discussion and plan.
The following CT scan depicts a thin frontal bone and large frontal sinus. In this type of setting, a Type 3 forehead reconstruction is undertaken.

 In type 3 forehead reconstructions, the prominent section of frontal bone is removed and setback. It is secured back into it’s new position with titanium plates and screws.
In type 3 forehead reconstructions, the prominent section of frontal bone is removed and setback. It is secured back into it’s new position with titanium plates and screws.
It is important to note that the frontal sinus can vary significantly between individuals. In some individuals the sinus is rudimentary. It is also the norm for one side of the sinus to be very different to the other side. This is shown above in the CT scan cross section image.
Pre surgery CT image of a patient presenting for brow bone reduction:


Post surgery CT image of the same patient after Type 3 brow bone reconstruction with complete correction of brow bone prominence


In Type 3 forehead reconstructions, it is critical that the frontal bone segment is removed with precision and within the confines of the frontal sinus boundaries in order to avoid injury to critical structures. Dr Reddy does this by undertaking careful preoperative CT planning to determine the exact boundaries of the sinus. During the surgery, It is important that the frontal sinus is also managed very carefully in order to minimise the risk of longer term sinus related sequela. The following intra-operative photos highlight the various steps involved in type 3 forehead reconstruction surgery.
Type 3 Forehead Reconstruction Gallery
Following bone setback and fixation, and careful management of the sinus, the forehead tissues are repaired, ensuring good brow position and symmetry.
Warning viewer discretion is advised
- Expert Advice
- Personal Approach
- Highly Respected
SYDNEY & CENTRAL COAST PLASTIC SURGEON
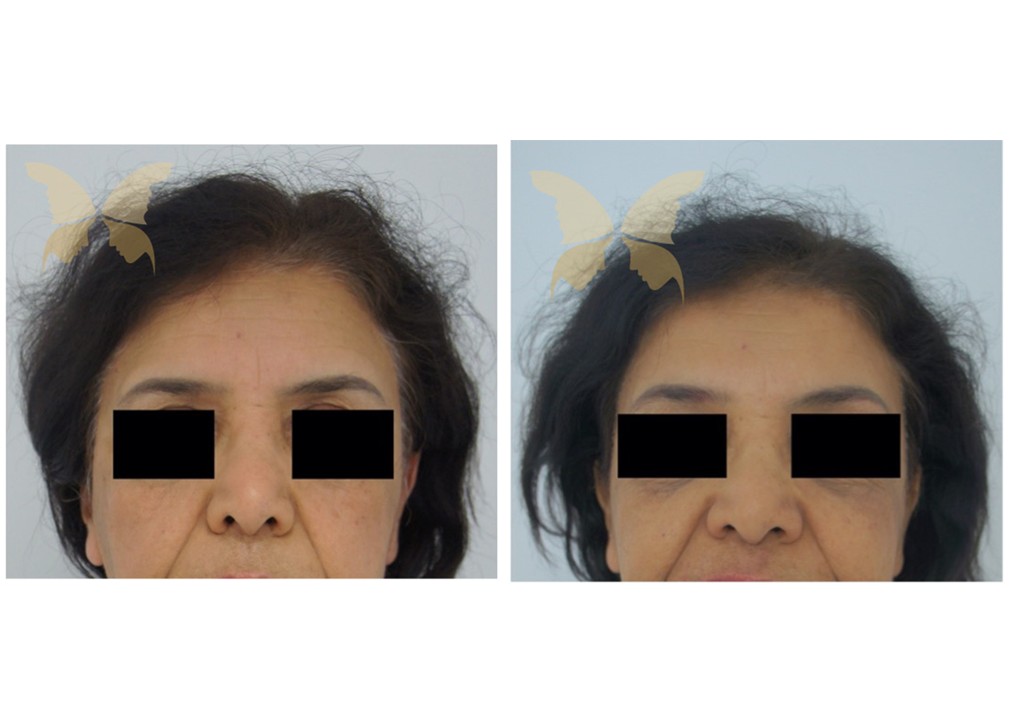
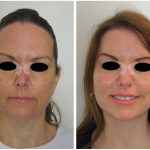
Forehead And Brow Prominence Reduction Gallery
Brow Lifting and Hairline lowering in Facial Feminisation Surgery
One also needs to consider the shape of the brow when discussing facial feminisation. An aesthetically ideal female brow has certain characteristics. The female brow is typically described as having a gentle upward curve as it continues outwards, the so-called “arched brow”.
This is in contrast to a male brow, which typically rests lower and more horizontally. Achieving a more arched brow can be achieved by undertaking a brow lift procedure. You may undertake brow lift surgery via a variety of methods. Typically, this is undertaken via a hairline incision.
This approach also enables access to the frontal bone if a brow bone reduction procedure is undertaken. Similarly, if a hairline lowering procedure is undertaken, this may also be performed via the same incision.
Specific techniques in incision planning are critical in undertaking a hairline approach. The incision blade must be angled appropriately to ensure the least disruption to hair follicles, leading to maximal hair growth penetration through the incision and an optimal well-concealed incision line.
Once the incision is made, forehead tissues are freed up to the level of the brow to enable adequate mobilisation and manipulation of the brow. It is also important that the tissues are freed up in a controlled manner so that over-elevation of the inner portion of the brow does not occur. This can lead to an undesirable, unnatural “surprised look”. The process of freeing up the brow also needs to be undertaken carefully to avoid any injury to the temporal branch of the facial nerve so that brow movement is also preserved. Once the brow has been freed up and elevated to the desired level, the tissues are secured into position. This can be undertaken with medical anchors or deep tissue sutures.
When viewed from in front, a male face tends to have an ‘M’ shaped hairline, whilst a female face tends to have more of an ‘O’ shaped hairline. Therefore, the feminisation of the face often entails a hairline lowering procedure to reduce forehead show and restore hair distribution in the upper outer aspect of the forehead.
Through his extensive experience with hairline lowering procedures, Dr Reddy has developed his own novel method of hairline lowering to specifically help address male pattern hairlines for the purposes of facial feminisation.
The alternative approach to restoring hair in this region is by way of hair transplantation. There are advantages and disadvantages of each approach, and Dr Reddy will routinely discuss these issues with you as part of the decision-making process.
Hairline Lowering Gallery
As one can see, feminising the upper third of the face may entail addressing one or more of the above-mentioned areas to transition towards a more natural-looking feminine face.
Rhinoplasty in Facial Feminisation Surgery
Various features typically characterise a female nose when compared to a male nose. A more feminine nose often exhibits the following distinguishing features:
- A slightly concave profile to the nasal bridge
- Narrower nasal bridge
- Narrower nostrils
- Smaller nose relative to the rest of the face
- A slightly upturned nasal tip
- The glabella angle (between forehead and nose) tends to be more obtuse
These distinguishing features are depicted in the images below.
Therefore, your surgeon should have a good understanding of these differences so that they can employ that appropriate measures and techniques during your rhinoplasty procedure to help ensure that a more feminised nasal shape is achieved. Please click here to read more information about rhinoplasty.
Facial Fat Grafting and Cheek Augmentation in Facial Feminisation Surgery
Another aspect of the mid-face that needs to be considered is the contour and prominence of the cheekbone region. A female face historically is described as having a rounder and softer contour in the cheekbone region. This contrasts with the more squared-off appearance that a male face often exhibits in the mid-face region. This is highlighted in the following images:
Achieving appropriate contour in the cheekbone region during facial feminisation surgery can be achieved through volume augmentation or cheekbone repositioning. Volume augmentation can be effectively achieved with facial fat grafting, malar implants, or the use of dermal fillers.
Facial fat grafting can play a vital role in achieving softer contours in the under-eye and cheekbone regions. When compared to dermal fillers, facial fat grafting has the significant advantage of producing long-lasting results. Some individuals also report improvement in skin quality and skin texture through the stem cell effects of fat grafting. To read more about facial fat grafting, please click here.
If one considers the lower third of the face, there are again various aesthetic ideals that distinguish a female face from a male face. A female face is often described with the following:
- A shorter upper lip with a slight upturn
- Upper teeth show
- Less prominent chin
- Less width to the lower jaw
- Less prominence to the angle of the jaw
Achieving a result that approaches the aesthetic ideals of a female face can therefore entail surgery to address these above areas.
Lip lift in Facial Feminisation Surgery
If one considers the lip region, one can achieve a more feminine appearance by undertaking a lip lift procedure. The procedure has the effect of reducing lip length and producing more upper incisor (teeth) show. This is undertaken by incorporating a well-concealed incision in the crease under the nose. The procedure is typically performed under local anaesthesia in a clinic setting without requiring hospital admission. Alternatively, it can be performed in a hospital at the same time as other facial feminisation procedures. To read more about lip lift surgery, please click here.
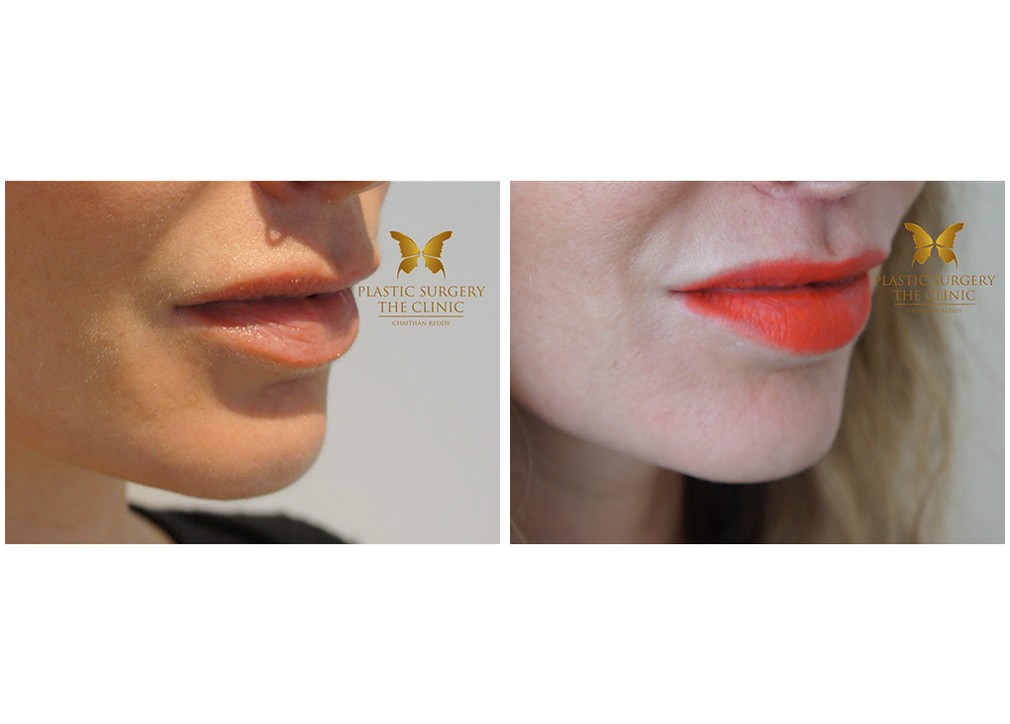
Lip Lift Before And After Gallery
Chin reduction and jaw reshaping in Facial Feminisation Surgery
In regards to the chin, achieving a more feminine facial profile typically entails reducing chin prominence. Various measurements comparing chin position to the rest of the facial profile (and nose) are undertaken to determine whether one’s chin position needs to be adjusted.
Various techniques are described to determine the ideal chin position, particularly if one compares the ideal position in a male vs female.
One well-known technique compares chin position to lower lip position. In a male, the chin ideally sits in line with a vertical line drawn vertically through the lower lip margin. This contrasts with the ideal chin position in a female, which sits slightly behind this vertical line. This is depicted in the diagram below.
However, it is important to note that this assessment tool should be taken as a guide only as other parameters, including important anatomical factors, such as skeletal shape and teeth position, need to be accounted for. Your surgeon must also be familiar with the other methods of determining the ideal chin position so that all of the relevant factors are considered, rather than relying on the lower lip position alone to determine the ideal chin position.
If chin projection is to be reduced, this can be undertaken by shaving back the underlying bone. This is feasible, providing only a small reduction is required. Larger chin reductions require repositioning of the bone itself by way of a sliding genioplasty procedure. You can access further information about sliding genioplasty here. This is depicted below.
Both chin projection and width can be reduced to create a more tapered appearance to the chin. There are two main approaches to achieving this result. The choice of procedure will depend on the thickness of the chin bone, the position of your teeth, and the amount of reduction desired. The bone may either be trimmed away and contoured. If this is not feasible or a more significant change in shape is desired, then a central segment of the chin bone may be removed, and the adjacent segments moved closer together to create a narrower chin. This is depicted in the image below.
Dr Reddy will be able to advise you on what may be required and which procedure will be feasible in achieving appropriate correction of your chin position.
Lower jaw shape and width
The remaining aspect that needs to be considered in facial feminisation assessment of the lower third of the face relates to the shape and width of the lower jaw.
In females, when the jaw is viewed from side-on, the angle of the lower jaw is typically more obtuse, with less backward projection of the jaw. This is shown in the diagram below.
Achieving the above usually entails shaving down the back surface of the lower jaw. This can be performed via incisions inside the mouth.
When the face is viewed from the front, the male jawline tends to be wider, with a more prominent jawline. In some individuals, feminising the face may therefore involve reducing the width of the lower jaw. Dr Reddy can do this by shaving down the outside surface of the lower jawbone. This can also be performed by placing incisions inside the mouth.
When a more aggressive reduction is required, the ‘mandibular angle’ bone segment may be removed by very carefully undertaking precise bone cuts. This is relatively difficult operation due to the limited access that is available to get to the back of the lower jaw. Furthermore due to the presence of important anatomical structures in the area, Dr Reddy undertakes these procedures after determining the exact location of the cut based on your pre-operative CT scans. As part of Dr Reddy’s planning, custom made models of the lower jaw can also be manufactured. This is shown below.


In individuals requiring even more narrowing of the entire lower jaw, a procedure known as V-Line surgery may be undertaken. This will not only correct a broader lower face shape, but can achieve a highly tapered chin. When V-line surgery is undertaken, the bone along the entire length of the lower jaw is removed in a planned manner to achieve a narrower and more feminine lower face shape.
The following images depicts the intra-operative appearance of the tapered chin bone achieved following V-line surgery as well as the segments of bone removed along the entire length of the lower jaw.


It is important that surgeons undertaking such procedures have extensive experience with lower jaw surgery and anatomy. Based on Dr Reddy’s experience as a dentist and in maxillofacial procedures, and also having undertaken several hundred lower jaw surgeries over the past two decades, he will be able to discuss the various lower jaw surgery options with you so that a suitable treatment plan is formulated specifically for your needs.
In some individuals, this type of bone shaving procedure is not required or not preferred. In these cases, you may achieve a reduction in lower jaw width by thinning the muscle (masseter muscle, also known as the clenching muscle). Muscle thinning can be achieved non-surgically with anti-wrinkle injections. There are advantages and disadvantages of each approach, and Dr Reddy will discuss these options with you in further detail during the consultation process.
Face & Neck Lift In Facial FeminisationWhen undertaking various lower jaw bone reduction procedures in facial feminisation, it is essential to consider the impact of such changes on the overlying soft tissues. When the lower jaw bone is reduced in width or the chin bone is reduced in prominence, the skin and soft tissues will typically settle downwards, as the shelf of bone to support these tissues are reduced. Another reason the skin and tissues tend to shift downwards to some degree is that in reducing the bone, the tissues are detached from their bony attachments. Whilst the tissues do reattach, some degree of shift is sometimes unavoidable. Depending on the degree of bony reduction and the quality of your skin tone, a lower face or neck lift procedure may be required to address these changes. This typically involves tightening the underlying musculature (platysma muscle or SMAS) to resuspend the tissues in a more favourable position.
You can find more information about lower face and neck lift surgery here.
Why choose our clinic?
- Having an experienced facial feminisation surgeon in Australia
- Individualised approach based on your desires with natural looking feminised results
- An inherent goal to achieve a feminised result rather than simply a technical result
- Comprehensive after care and advice
- No need to travel overseas, minimising travel related surgical risks and aftercare difficulties
- A dedicated clinic team and operating theatre team familiar with facial feminisation
- Offering facial feminisation to interstate and international patients
- Kindly recommended by past patients
Please feel free to reach out when you are ready to embark on your facial feminisation journey. Dr Reddy has a great deal of respect for these procedures and understands that this can be a critical decision in your life during the transition process.
We pride ourselves on providing a caring and well-supported environment during the consultation, surgery, and aftercare process. We understand that many individuals may travel overseas to have these procedures for cost reasons. Whilst having surgery overseas may appear to be a cheaper option, in our experience, significant unexpected costs tend to arise for patients when they have to address complications once back in Australia. An important aspect to consider is that these procedures require strict attention to detail, experience, and readily available aftercare, particularly during the first few months after surgery. Surgery in Australia also ensures compliance with the necessary surgical standards and strict hospital sterilisation and accreditation processes.
Given the life-changing nature of these procedures and stringent aftercare requirements, we pride ourselves on ensuring thorough and readily accessible post-surgical care over the longer term.
What is also critical is having a surgeon that has an in depth understanding of the fundamental differences between male and female facial presentation. This goes beyond simply being able to undertake the technical aspects of surgery, but rather having a confident appreciation of how underlying changes to the facial skeleton affect the facial framework and overlying soft tissues. And, how complementing the skeletal surgery with soft tissue procedures can have a profound impact on achieving a feminine face.
Having a highly qualified facial feminisation surgeon in Australia that has extensive experience in facial bone surgery and an in depth understanding in facial beautification procedures becomes paramount in achieving not just a technical result but a feminine result in keeping with the desired endpoint. Dr Reddy not only has extensive experience in facial bone and lower jaw surgery, but has an extensive track record in facial feminisation soft tissue procedures such as browlifting, hair-line lowering, lip lift, cheek augmentation, facelifting and feminising rhinoplasty.
We look forward to being involved in your surgical care and would be priveleged to be involved in your facial feminisation journey.